Certified Registered Nurse Anesthetists: An Overview
Certified Registered Nurse Anesthetists are independent anesthesia professionals that work in all models of anesthesia delivery, in all settings, and with diverse patient populations.
FAQs
Are CRNAs capable of providing independent anesthesia services?
CRNAs have always independently provided the full range of anesthesia services. In recent years, the number of CRNAs providing independent services has increased to nearly half (42.5%) of all CRNAs.
Local facilities can choose from a number of different anesthesia delivery models based on their communities unique attributes. All models have been repeatedly demonstrated to be equally safe, and they range from "solo" models, to collaborative teams (focusing on teamwork and competency rather than "supervision") to a model known as "medical direction" where 1 anesthesiologist oversees the anesthetic delivered by 4 CRNAs.
The medical direction model is derived from billing requirements, is not a standard of care, and while safe, does represent a higher cost for patients and facilities and often requires a subsidy.
Can surgeons or physicians doing procedures be held liable for CRNA practice?
No. You can find the surgeon immunity section of Arizona Revised Statute 32-1634.04 here.
Do CRNAs train to administer all types of anesthesia for surgical patients?
Yes. The Council on Accreditation requires extensive experience in all areas of surgery. While there are individual variations in training and experience, all CRNAs receive a broad baseline of education and experience.
Are CRNAs nationally board certified?
Yes, all CRNAs are required by state and federal law to be nationally board certified by the only recognized body in the United States for certifying CRNAs, the National Board of Certification and Recertification of CRNAs.
What's the real difference between physician anesthesiologists and CRNAs?
Both professions offer similar, and often overlapping, services. Broadly, while they have different backgrounds, both professions study the same physiology, pathophysiology, pharmacology, and anesthetic management. Of course individual professionals gain experience in different practice areas, and while all CRNAs and anesthesiologists are generally well trained, they are not all the same - which accounts for regional differences in practice models.
How do CRNAs combat the opioid crisis?
CRNAs with subspecialty training in chronic pain injections and management play a key role in reducing opioid use, by eliminating pain and thus the need for continue opioids. This emerging area of practice is rapidly growing to address a national epidemic.
Where can I find the updated CRNA Scope of Practice; Physician and Surgeon Immunity; in Arizona Statute?
You can find Arizona Revised Statute 32-1634.04 here.
Is Arizona an “opt out state” i.e. has Arizona removed the requirement from CMS to have CRNAs supervised?
I’m not getting AZANA emails. What should I do?
Confirm you are an AANA member with your address listed in Arizona.
Confirm the email account you are checking is the one associated with your AANA profile. Some organizations have firewalls, personal emails may have fewer issues.
Check your Spam, Junk and Promotions folders.
Be sure that the following emails are added as contacts:
If you are still having issues, please contact desirae@azcrna.com.
Suited to Meet Today’s Healthcare Challenges
Certified Registered Nurse Anesthetists (CRNAs) have been providing anesthesia care to patients in the United States for more than 150 years. CRNAs collaborate with surgeons, anesthesiologists, dentists, podiatrists, and other qualified healthcare professionals to deliver safe, high-quality, and cost effective patient care in virtually every healthcare setting.
When anesthesia is administered by a nurse anesthetist, it is recognized as the practice of nursing; when administered by an anesthesiologist, it is recognized as the practice of medicine. While all anesthesia professionals deliver the same anesthetics, anesthesia care delivered by a CRNA is especially well-suited to meet the needs of today’s changing and challenging healthcare environment. Key benefits of CRNA-delivered anesthesia care include:
Most cost-effective anesthesia care model
Ensures access to anesthesia in medically underserved communities where surgical, obstetric, and trauma services otherwise would not be available
Consistently provides a safe anesthesia experience and quality outcome for each patient
Extensive preparation for handling emergency situations
Healthcare team members count on CRNAs to provide services beyond anesthesia care
CRNAs offer broad services and and training costs are significantly lower for state budgets . Image courtesy of uiowa.edu
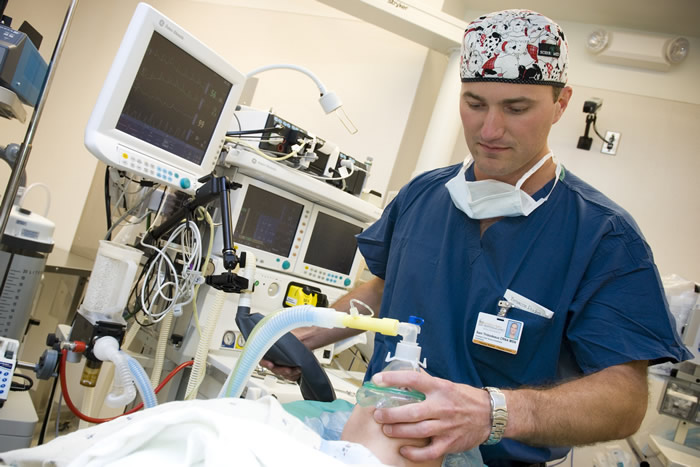
Independent CRNAs operate independently in front-line surgical hospitals throughout the world. Image courtesy of army.mil
CRNAs: Safe Care
Like all healthcare professionals, a quality outcome for each patient is the main mission of the CRNA. Like all professionals, nurse anesthetists take steps every day to consistently deliver on this mission. In the U.S., deaths attributed to anesthesia during surgery are extremely rare, occurring approximately once in every 250,000-300,000 anesthetics provided.
Several landmark studies confirm that CRNAs achieve the same level of safety and quality as their physician counterparts. In fact, researchers consistently find anesthesia care is equally safe whether provided by a CRNA working alone, an anesthesiologist working alone or a CRNA working with an anesthesiologist.
Not surprising, laws, rules or regulations in well over half of all states do not require physician supervision of CRNAs. And 17 states have opted out of the federal Medicare requirement that calls for physician supervision of CRNAs. In the operating room, surgeons quite properly defer to nurse anesthetists as the experts in anesthesia care, regardless of whether their state requires physician supervision.
CRNAs: Accessible Care
Affordable healthcare available to everyone remains a primary goal of today’s healthcare system, even with the influx of more and more customers. CRNA-managed anesthesia care allows healthcare providers to prevent gaps in access and continue to deliver much-needed services in thousands of communities. When access is the problem, CRNA-administered anesthesia care is often the first, best solution:
Prescott, Yuma, Show Low, Payson, Nogales are all examples of communities which rely on CRNA-only care to ensure accesible surgical services. Image courtesy of Arizona Rural Health Assocaition.
CRNAs are the primary providers of anesthesia care in rural America.
In some states, CRNAs are the sole anesthesia professionals in nearly 100 percent of rural hospitals.
CRNAs provide tens of millions of rural Americans access to surgical, obstetrical, trauma and pain management services. This means individuals don’t have to travel long distances to receive needed care. Without those services, local hospitals in rural communities could not exist. And without local rural hospitals, the viability of rural communities would be very much at risk.
CRNAs are the primary anesthesia professionals in many medically underserved inner-city communities.
CRNAs provide the majority of anesthesia care in the Veterans Administration and U.S. military.
And for years, CRNAs have been the predominant providers of anesthesia services to maternity patients, providing needed anesthesia during labor and delivery. CRNAs monitor fetal status prior to analgesic or anesthesia intervention, and are available to help with neonatal assessment and resuscitation.
CRNAs: Educated Care
Dr. Shari Burns, CRNA EdD, leads the DNAP completion program at MIdwestern University. Image courtesy of Midwestern.edu.
Patients, caregivers and administrators must have confidence in the professionals providing healthcare. As highly educated, advanced practice registered nurses, CRNAs deliver anesthesia to patients using the same procedures as physician anesthesiologists. With an average of three and a half years of critical care experience before entering a nurse anesthesia program, CRNAs are well prepared to respond appropriately in emergencies. They are the only anesthesia professionals with this level of critical care experience prior to beginning formal anesthesia education.
Additionally, nurse anesthetists attain seven to eight years of education, training and work experience. Today’s CRNAs enter the workforce with a master’s or doctoral degree. CRNAs must receive their master’s or doctoral degree from a program accredited by the Council on Accreditation of Nurse Anesthesia Educational Programs (COA). By 2025, all CRNAs will receive a doctoral degree from a program accredited by the COA.
During surgery, often the patient’s life rests in the hands of their anesthetist. This enormous responsibility requires CRNAs to use every aspect of their education and training, nursing skills and scientific knowledge. CRNAs are qualified to administer every type of anesthesia to all types of patients in any healthcare setting. Nurse anesthetists deliver comprehensive care using all accepted anesthetic techniques including general, regional, sedation, local and pain management.
CRNAs: Collaborative Care
Patients, caregivers and facility administrators expect their healthcare team to work together. CRNAs are prepared to collaborate with all members of the patient care team including surgeons, endoscopists, radiologists, podiatrists, obstetricians, anesthesiologists, nurses, technicians, other specialists and operating room personnel.
In today’s fast-paced healthcare environment, patients and the patient care team also look to their CRNA to fill roles beyond administering anesthetics.
CRNAs are responsible for patient safety before, during and after anesthesia.
CRNAs sustain a patient’s critical life functions throughout surgical, obstetrical and other procedures.
CRNAs are uniquely prepared to assess, identify and manage the care of patients suffering from acute and/or chronic pain.
CRNAs select and administer other types of drugs to preserve life functions.
CRNAs analyze situations and respond quickly and appropriately in emergencies.
And CRNAs provide that special spirit of caring that is unique to all nurses.
Read real-life stories of CRNAs helping America’s healthcare providers deliver quality care to more people at lower costs.
CRNAs: Cost-Effective Care
As U.S. healthcare providers brace to handle providing care to some 30 million new customers, managing costs is of paramount concern. The challenge – find ways to improve patient access to safe, quality care without over-burdening the system.
Enter the CRNA. These trained professionals deliver the same safe, high-quality care as other anesthesia professionals but at a lower cost. In fact, a landmark study published in 2010 found that the most cost-effective anesthesia delivery model is a CRNA working as the sole anesthesia provider. Because Medicare pays the same fee for anesthesia services provided by a CRNA, an anesthesiologist, or both working together, the higher compensation of the anesthesiologist is borne by the hospital, healthcare facility or patients. Legislation passed as part of the Affordable Care Act promotes coverage of CRNA services within their scope of practice, so health plans support a competitive, high-quality healthcare marketplace. And most managed care plans recognize CRNAs for providing high-quality anesthesia care with reduced expenses to patients and insurance companies.